Multiple sclerosis (MS) is a lifelong neurologic disease affecting the central nervous system and resulting in demyelination and axonal loss over time. Symptoms are widely variable and often involve motor and sensory impairment, vision loss, gait disturbance, cognitive dysfunction, and fatigue. Furthermore, MS is a disease common to women of childbearing age, with 70% of patients being women and with 90% of patients presenting between the ages of 15 and 50.1 Family planning must be taken into account at time of diagnosis and when discussing which disease modifying agent to employ. Accurate knowledge and understanding of family planning issues is important for best outcomes.
The relationship between pregnancy and relapse outcomes is complex and might not be fully understood by many patients. Many studies have shown that pregnancy can have a protective effect against MS relapses, although the mechanisms underlying this phenomenon are still being studied. The Pregnancy in Multiple Sclerosis (PRIMS) study evaluated 227 women with MS from 1 year prior to pregnancy until 2 years after delivery and found that the risk for relapse decreased by about 70% during the third trimester but increased by twofold in the 3 months postpartum compared with the risk for relapse during the prepregnancy year.2,3 Furthermore, the long-term favorable effects of pregnancy on patients with relapsing-remitting MS have been established by several studies, demonstrating a lower risk for reaching an Expanded Disability Status Scale of 6.0 and thus a decreased possibility of needing an ambulatory device.4
Education about peripartum concerns is also paramount. In a study of 461 women with MS, there was a higher rate of caesarian section; however, these findings represented a concurrently higher rate of planned, rather than emergency, caesarian sections,5 a finding that might reflect an overly cautious approach. Previous practice advocated for caesarian sections to avoid pelvic floor trauma and thus exacerbation of preexisting urinary frequency and bladder control issues; however, it was shown in a study of 273 women in 2006 that urinary incontinence postpartum was more related to duration and severity of MS and not method of delivery.6
Similarly, accurate knowledge about environmental and genetic influences on MS is crucial for informed family planning considerations. Overall, MS is not considered a principally hereditary illness, and the risk for MS in the general population is approximately 0.1% compared with the risk in children of an affected parent, which is approximately 3%. For dizygotic twins, the risk for the second twin developing MS is about 4%, and for monozygotic twins the risk is about 30% over their lifetime.7,8 In terms of environmental risks, there was previous concern over use of oral contraceptives, which has been dispelled by studies showing both no effect and even possible association with a milder MS course. It is also important that women with MS and their offspring are not dissuaded from using oral contraceptives over concerns of developing MS.9,10
Furthermore, familiarity with pregnancy risks with MS disease-modifying therapies (DMTs) can lead to safe family planning practices. Current safety data is only based on animal studies and/or human observational cohorts and registries. Of the 13 approved medications, glatiramer acetate has shown no evidence to date of any danger to fetuses, but there is possible evidence for toxic effects with the other medications in animal and/or human studies, including known harm with teriflunomide in animal studies for which there is an absolute contraindication during pregnancy.11 Patients on certain DMTs must be aware that they might need to undergo a washout period prior to becoming pregnant. Moreover, it is equally important for women to know that it is safe to receive intravenous methylprednisolone (IVMP) for treatment of MS exacerbations during the second and third trimesters, and with caution during the first trimester. For breastfeeding women it is recommended to “pump and dump” for four hours after IVMP treatment.1,5,12
Use of DMTs then necessitates education about consistent contraception and safety while breastfeeding. For example, while there is no evidence that glatiramer acetate is absorbed into a newborn’s gastrointestinal tract to any significant degree, safety has not been established. There was one study of interferons and breast milk that showed that it is present in extremely small amounts,13 and natalizumab is detectable in breast milk but might not be absorbed by an infant. All three oral MS medications (fingolimod, dimethyl fumarate, teriflunomide) are known to be detectable in animal breast milk.11 In terms of relapse risk, the decision to breastfeed versus restarting MS therapy after delivery is complex, as patients must weigh increased risk for postpartum relapse off of therapy with the putative protective benefits of breastfeeding. However, exclusive breastfeeding typically requires a patient to remain off of DMTs, and thus the risks and benefits of these highly personal decisions must be made on an individual basis.14
Given these complexities, our objective was to delineate which misconceptions might exist within the female MS population with regards to family planning, pregnancy, breastfeeding, MS genetics, and medication safety through a pilot study.
Methods A questionnaire with topics pertaining to MS and pregnancy was created by three neurologists, two of whom are MS specialists. The questions ranged from simple to more esoteric with the intention of determining the full spectrum of patient knowledge. The questionnaire was first reviewed for content and appropriateness by an interdisciplinary team at the MS
center. Questionnaires were then distributed to patients who were willing to participate and finished anonymously. Upon completion the participants were given an educational answer key. The project was reviewed by the Institutional Review Board and deemed exempt.
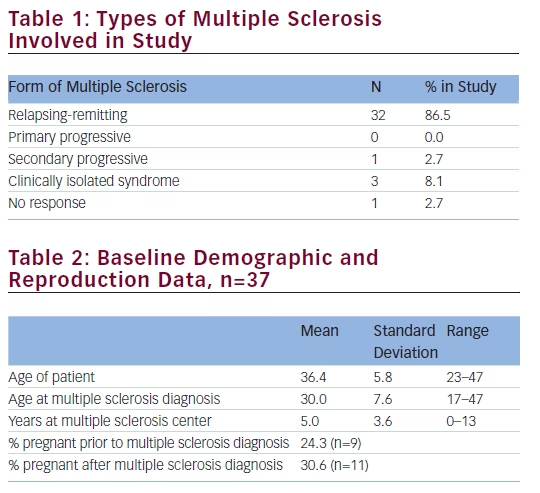
We recruited all willing patients who met our inclusion criteria seen at the MS center every clinic day during a 2-month time window. Thirty-seven female patients of childbearing age (which, for the purposes of the study, was defined as ages 18 to 50) with confirmed MS or clinically isolated syndrome (CIS) were selected to participate from a single MS center in New York City. All types of MS were included but only patients with relapsing remitting, secondary progressive, and clinically isolated syndrome participated (see Table 1). No patients with primary progressive MS completed the survey. The status of being on a DMT at the time of the study was not a basis for exclusion. Ability to speak and read English was also an inclusion criterion.
Baseline demographics and reproductive history were collected and included the following: number of years since MS diagnosis, number of pregnancies before and after MS diagnosis (including terminations or miscarriages), type of MS, the number of total adverse events during pregnancy, consistent use of birth control while on a DMT, and patients’ primary source of MS information (including their MS care provider, patient care organizations, and the Internet).
The knowledge-based questionnaire (see Figure 1) comprised 22 questions divided into four main categories: 1) the effect of pregnancy on MS; 2) the effect of MS on pregnancy; 3) medication safety during pregnancy and breastfeeding; and 4) the effect of MS on offspring. Patients were given an educational answer key after completing the questionnaire.
Using Excel© and Stata© data analysis and statistical software, the frequency of answers in the demographic section was calculated to provide a mean with standard deviation and a range. The number of correct answers was also calculated and reported as frequency and
percentage, including the average overall score as well as score on individual questions. The overall scores were compared for statistical significance using an independent sample t-test between responders who had been pregnant since MS diagnosis and those who had not been pregnant. A p value of <0.05 was considered statistically significant.
Questions were grouped into four major topic categories for further analysis. Based on the demographic data supplied, we also completed subgroup analyses based on whether the patient had been pregnant since MS diagnosis and compared test results to those of patients who had not been pregnant since diagnosis. Given the small sample size in these subgroup analyses, we used a nonparametric Wilcox rank sum test to determine statistical significance between scores and to generate a p-value.
Results
The average age of patients surveyed was 36 (range 23–47 years). The mean age at the time of MS diagnosis was 30. The average number of years since MS diagnosis was 6.7. Eleven patients had been pregnant after MS diagnosis, 30.6%, and nine patients had been pregnant prior to diagnosis, 24.3% (see Table 2). Of those who had been pregnant at any time, 8% (n=3) reported an adverse fetal outcome when pregnant; however, reasons for the adverse outcomes were not provided. In terms of where patients reported obtaining information about their disease, 78% reported that their MS care provider was their main source of information.
Patients answered an average of 32.8% (standard deviation [SD]±20.3) of questions correctly overall. In the subgroup of patients who had been pregnant since their MS diagnosis, there was a slightly higher average score of 40.5% (SD±24.7) correct. Those who had not been pregnant since diagnosis overall had an average of 31.3% (SD±17.9) correct. However, the difference in test scores between the groups was not statistically significant, p-value 0.21.
The four main categories of knowledge were analyzed for correctness, and the largest area of deficit pertained to the effect of MS on reproduction, with an average of 27.7 percent (SD±10.1) of questions answered correctly (see Table 3). When patients who had been pregnant after MS diagnosis were compared with those who had not been pregnant, answering 32.0% (SD±25.3) and 27.2% (SD±28.8) correct, respectively, the difference in test scores was not statistically significant, p-value 0.53. For questions related to the effect of pregnancy on MS disease course, the overall percentage correct was 34.0 (SD±25.4). Patients who had been pregnant after MS diagnosis showed a trend toward much higher scores in this category, 44.3% (SD±17.1) correct, while those who had not been pregnant averaged 31.4 (SD±20.2) on these questions. Again, the difference between groups was not statically significant, p-value 0.06.
On questions pertaining to medication safety, an average of 35.9% (SD±9.2) were answered correctly, and only 21.0% of responders knew that relapses could be treated with steroids during pregnancy. In subgroup analysis of participants who had been pregnant since MS diagnosis, 50.0% answered this question correctly. Furthermore, on questions pertaining to the safety of breastfeeding while on DMTs, only 46.0% correctly responded that most MS immunotherapeutic agents were not safe. Overall comparison of patients who had been pregnant after MS
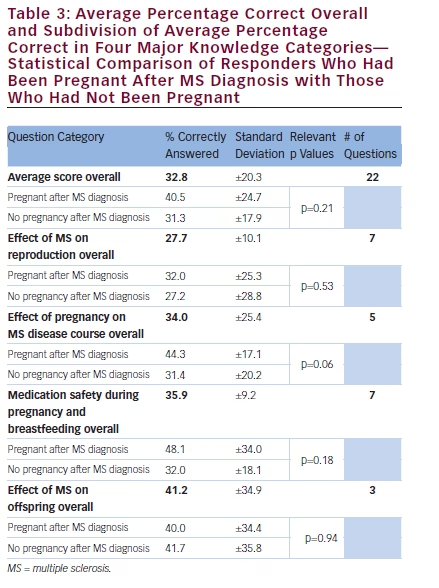
diagnosis to those who had not been pregnant showed a difference in scores of 48.1% (SD±34.0) versus 32.0% (SD±18.1), respectively, on medication-related questions. However, the difference between the two groups was not ultimately statistically significant, p-value 0.18.
From a family planning standpoint, only 37.8% of respondents correctly answered a question affirming the importance of birth control while on DMTs. Of those participants who themselves were on DMTs, 34.0% reported that they did not consistently use some form of birth control. Concurrently, over half of responders, 51.5%, knew that oral contraceptives do not carry an increased risk for development of MS.
Questions pertaining to the effect of MS on offspring yielded the highest subcategory score with 41.2 (SD±34.9) answering correctly. Only on these questions did patients who had not been pregnant since MS diagnosis score overall higher than women who had been pregnant, 41.7% (SD±35.8) versus 40.0% (SD±34.4), respectively. However, the difference was not statistically significant, p-value 0.94. On a particular question asking respondents if they agreed that daughters of women with MS have a 10% lifetime risk of developing the disease, 38.9% answered “no” correctly, with 27.8% saying that they thought this was true and another 33.3% uncertain about the correct answer. In terms of patients with MS carrying a moderately high risk of causing congenital malformations in their offspring, only 38.9% knew that this was incorrect, with an uncertainty answer of 55.6%.
Discussion
This pilot in essence reveals both limitations in patients’ knowledge and also serves as a “difficulty validation” on our survey instrument, as the questions were both clinically relevant and challenging to the correct degree. Using this questionnaire, we found that the majority of our population of female MS patients of childbearing years did not have a sufficient understanding of many topics pertinent to reproduction. We identified a number of misconceptions related to significant reproductive topics, medication safety, and patient behavior in women with MS.
An area of relatively robust knowledge was the effect of MS on offspring. Large knowledge gaps were found, however, in the areas of disease effect on reproduction and medication safety during pregnancy and breastfeeding. Of particular concern was a low awareness of the need for birth control while on DMTs, with a concurrently low self-reported claim of effective use of contraception. Over half of responders knew that oral contraceptives do not cause MS, making the low use of birth control less likely to be attributable to a fear of its use. Furthermore, answers to questions about US Food and Drug Administration (FDA) safety categories reflected a poor understanding of this classification system. Education on the topic of pregnancy safety categories for DMTs could help to prevent adverse fetal outcomes. However, it is important to note that over the course of this study, there has been a plan to phase out the current FDA classifications and replace them with a more descriptive labeling system.16 Any future large cohort study will have to addend the questionnaire accordingly.
Knowledge gaps pertaining to the possibility of relapse treatment during pregnancy could lead to undertreatment of disease activity occurring during pregnancy. It is notable that patients who had previously been pregnant had a trend toward scoring better on this question, suggesting that this health knowledge was acquired during pregnancy when it was most applicable. However, overall comparison of patients who had been pregnant since diagnosis to those had not been pregnant did not ultimately show statistically significant differences in scores.
Our study also identified patients’ misperceptions about negative effects of MS on pregnancy and offspring, which might discourage them from starting families. While some studies have shown a higher rate of assisted vaginal deliveries, for example requiring induction and slower progression of labor,5 there is evidence to suggest that mothers and newborns do equally well and do not have longer birth hospitalizations that non-MS counterparts, even when accounting for longer disease duration and increased disability.15
Our study has several limitations. As a single-center pilot study conducted in an urban area, our results might not be broadly generalizable to the MS population. An alternative explanation for the poor knowledge-based scores was that the questions were too difficult, rather than reflecting a genuine lack of reproductive education in this population. It should be noted that the population served by this MS center is a comparatively highly educated and health-literate group.
Conclusions
Our data identified patient misconceptions on a range of important reproductive topics related to MS. Use of similar knowledge assessments is practical for MS centers in order to identify education needs. Given that the majority of participants indicated that their MS practitioners are their primary source of information, it is critical that providers take the time to educate effectively their patients on issues of reproduction, prior to and after conception. We intend to replicate this study on a broad geographic cohort towards planning educational initiatives to address these needs. Future research in this area could evaluate the impact of pregnancy-related educational initiatives on improving reproductive health outcomes.







